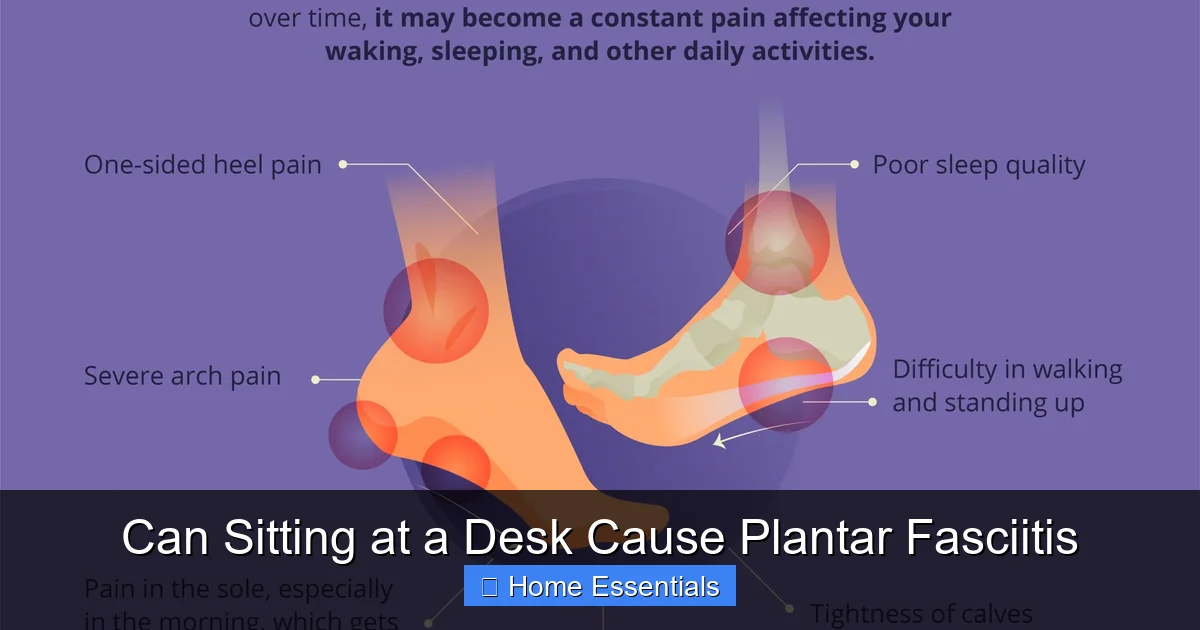
Can Sitting at a Desk Cause Plantar Fasciitis
Yes, sitting at a desk for long periods can indeed contribute to the development of plantar fasciitis. While often associated with standing or running, prolonged sitting leads to tightness in the calf muscles and the plantar fascia itself. When you finally stand or walk, this tight, shortened tissue is overstretched, causing micro-tears and the characteristic stabbing heel pain. The key is not just avoiding sitting, but managing your posture, footwear (or lack thereof), and movement breaks throughout the day to keep the tissue flexible and supported.
Key Takeaways
- Prolonged sitting tightens key structures: Sitting with feet flat or dangling shortens the calf muscles (gastrocnemius and soleus) and the plantar fascia ligament on the bottom of the foot, making them prone to injury upon standing.
- Poor sitting posture is a major culprit: Sitting with feet not flat on the floor or on tiptoes, crossing ankles, or using a footrest that forces plantar flexion (toes pointed down) keeps the fascia in a constantly shortened position.
- The “first-step” pain is a classic sign: The severe heel pain felt with the first few steps after sitting or lying down for a while is a hallmark symptom of plantar fasciitis triggered by inactivity.
- Ergonomics extends to your feet: A proper home office setup includes a chair height that allows feet to rest flat on the floor or a supportive footrest, promoting a neutral ankle position and reducing strain.
- Movement is non-negotiable prevention: Regular, short breaks to stand, walk, and perform simple calf and foot stretches are the most effective way to counteract the effects of sitting.
- At-home footwear matters: Wearing supportive shoes or sandals even while working at a standing desk or during breaks is critical; walking barefoot on hard floors on tight fascia is a recipe for pain.
- It’s a cycle of tightness and overload: Sitting creates tightness, which makes the fascia less able to absorb shock. Then, normal activities like walking to the kitchen overload this weakened, tight tissue, causing inflammation and pain.
📑 Table of Contents
- The Unlikely Connection: Your Office Chair and Your Heels
- Anatomy 101: What is the Plantar Fascia and Why Does it Hate Sitting?
- The Sitting Trap: How Your Desk Job Creates Tightness
- The Home Office Ergonomics: A Full-Body Problem with a Foot Solution
- Breaking the Cycle: Prevention and Management Strategies
- When to Worry: Red Flags and Professional Diagnosis
- Conclusion: It’s About Mindful Movement, Not Just Avoiding Chairs
The Unlikely Connection: Your Office Chair and Your Heels
When you think of plantar fasciitis, you probably picture a runner, a nurse, or a construction worker—someone on their feet all day. The idea that your comfy office chair could be a primary suspect in causing that excruciating stabbing pain in your heel with your first steps in the morning seems counterintuitive, almost backwards. But the science and clinical experience tell a different story. The very act of sitting still for hours on end is a potent recipe for creating the perfect conditions for plantar fasciitis to take hold. It’s not the sitting itself that directly injures the tissue, but what sitting *does* to the muscles and ligaments in your lower legs and feet. It’s a stealthy, slow-burn process of tightening and weakening that only reveals itself when you finally put weight on your feet.
Think of your plantar fascia like a big, strong rubber band running from your heel bone to your toes. Its job is to support your arch and absorb shock with every step. Now, imagine leaving that rubber band in a drawer, pulled taut and fixed in a shortened position for eight hours a day. Over time, it’s going to lose its elasticity. It becomes stiff, brittle, and less able to stretch when needed. That’s essentially what happens when you sit at a desk. Your calf muscles and the plantar fascia are held in a relatively fixed, shortened state. When you stand up, that stiff, shortened rubber band is violently stretched to its limit, leading to microscopic tears at its attachment point on the heel bone. This is the inflammation and pain we call plantar fasciitis. The connection is so strong that many patients with desk jobs report their worst pain after a long weekend of sitting or a vacation, not after a day of intense activity.
Anatomy 101: What is the Plantar Fascia and Why Does it Hate Sitting?
The Body’s “Bowstring”
To understand the sitting link, we need a quick anatomy lesson. The plantar fascia is a thick, fibrous band of connective tissue (a fascia) on the sole of your foot. It originates from the calcaneus (your heel bone) and fans out to attach to the bases of your toes. Its primary functions are to maintain the foot’s arch, absorb shock during gait, and assist in propulsion (the “push-off” phase of walking). It’s designed to stretch and recoil like a spring.
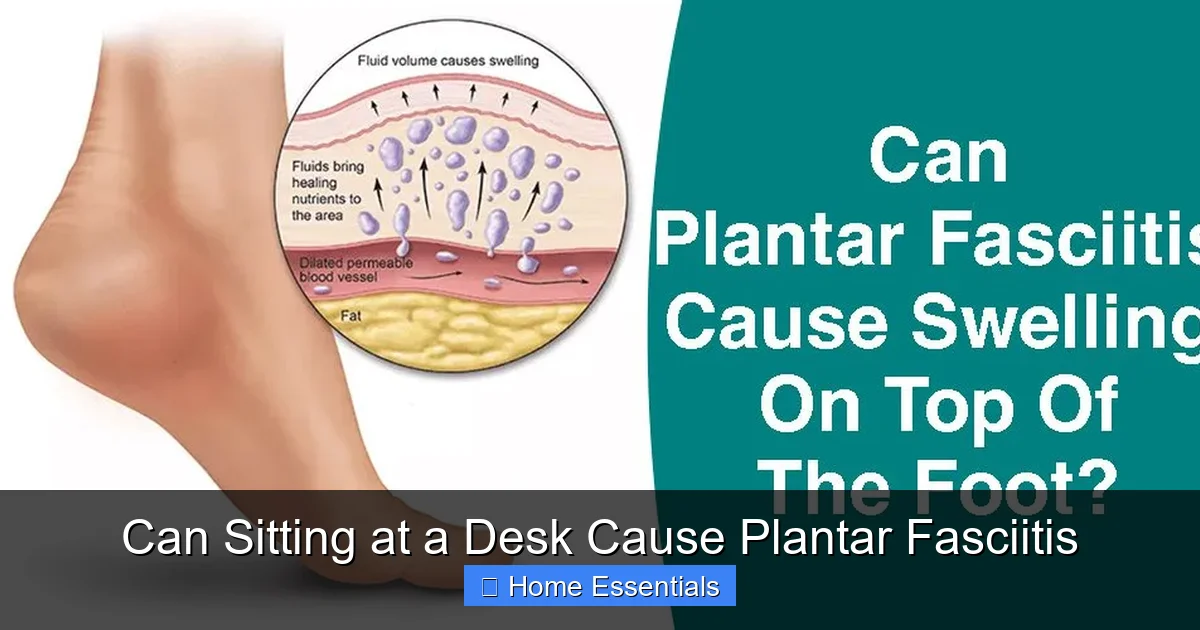
Visual guide about Can Sitting at a Desk Cause Plantar Fasciitis
Image source: baronactive.b-cdn.net
The Kinetic Chain: From Hip to Heel
The plantar fascia doesn’t work in isolation. It’s the final link in a kinetic chain that starts at your hip and includes your knee, ankle, and calf muscles. The two main calf muscles, the gastrocnemius (the bulky, visible one) and the soleus (deeper, underneath), merge into the Achilles tendon, which inserts directly into the heel bone—right next to where the plantar fascia starts. If your calves are tight, they pull on the Achilles tendon, which in turn increases tension on the plantar fascia. Sitting with your knees bent for long periods puts these calf muscles in a shortened, relaxed position. When you then stand, these tight muscles resist lengthening, placing extra strain on the plantar fascia to compensate. It’s a system-wide problem originating from your seated posture.
The Sitting Trap: How Your Desk Job Creates Tightness
Not all sitting is created equal. The specific way you sit at your desk dictates exactly how your foot and calf tissues are affected. Many common sitting habits are direct contributors to developing plantar fasciitis.

Visual guide about Can Sitting at a Desk Cause Plantar Fasciitis
Image source: verywellhealth.com
Feet Flat? Or Are They “Dangling”?
If your chair is too high and your feet don’t reach the floor, they dangle. This puts the ankle in a state of slight plantar flexion (toes pointed down). In this position, the calf muscles and Achilles tendon are shortened. Even if your feet *do* touch the floor, if you’re perched on the edge of your seat or have a tendency to rock back on your heels, you’re still engaging a plantar-flexed position. The ideal is feet flat on the floor (or on a footrest) with knees at or slightly below hip level, creating a neutral 90-degree angle at the ankle. This neutral position distributes weight evenly and keeps tissues at their natural resting length.
The Perils of the “Foot Tuck” and Crossed Ankles
Many people subconsciously tuck one foot behind the other ankle or cross their ankles while sitting. This actively forces the foot into plantar flexion and often inversion (turning inward). This not only shortens the calf and plantar fascia on that side but can also create an imbalance, pulling the foot out of alignment. Over hours, days, and years, this repetitive, abnormal positioning trains the soft tissues to adapt to a shortened state, setting the stage for pain when normal, neutral walking resumes.
Footrests: Friend or Foe?
A footrest can be a fantastic tool for ergonomics, but only if used correctly. A footrest that is too high or has a sloped, rocker-bottom design that forces your toes up (dorsiflexion) can be excellent. However, a common mistake is using a footrest that encourages you to rest the *top* of your foot on it, which again puts the ankle in plantar flexion. The goal is to have the entire sole of your foot supported on a stable surface, with the ankle in a neutral, relaxed position. If you find yourself pointing your toes to rest on your footrest, it’s the wrong height or shape for you.
The Home Office Ergonomics: A Full-Body Problem with a Foot Solution
Your workstation setup is the root cause. An improperly configured desk and chair force your entire body—including your feet—into poor postures. Addressing plantar fasciitis from sitting requires looking at the whole picture.

Visual guide about Can Sitting at a Desk Cause Plantar Fasciitis
Image source: sp-ao.shortpixel.ai
Chair Height and Seat Depth
This is ground zero. Your chair height must allow your feet to rest flat on the floor. If you’re short, a footrest is essential. If you’re tall, you may need a higher chair and possibly a footrest to prevent your knees from being lower than your hips, which increases shear force on the lower back and can indirectly affect gait. Seat depth matters too; if the seat pan is too long, it will press into the back of your knees, reducing circulation and potentially causing you to slide forward, losing that vital flat-footed support.
Desk Height and Monitor Placement
If your desk is too high or too low, you’ll compensate with your body. A desk that’s too high often leads to hunched shoulders and raised elbows, but it can also cause you to lift your feet off the floor or rock on your chair. A desk that’s too low causes you to slump forward, which can shift weight and lead to crossing legs or tucking feet under. Your monitor should be at eye level to prevent neck strain, which can cascade down the spine and affect pelvic tilt and, ultimately, leg and foot alignment during movement. For those using smart lighting to reduce eye strain, proper monitor ergonomics become even more important to avoid squinting and postural compensation.
The Standing Desk Consideration
Many people switch to a standing desk to combat sitting, and this can be a great strategy. However, it introduces its own set of risks. Standing still for hours is just as bad as sitting. The key is *movement* and *transition*. A sit-stand desk is ideal. The protocol is to start with short standing intervals (15-20 minutes) and gradually increase. Crucially, when standing, you must wear supportive shoes. Standing barefoot or in flimsy socks on a hard floor while your fascia is still tight from the morning will aggravate it instantly. Consider an anti-fatigue mat for cushioning. Also, ensure your standing posture is correct—weight evenly distributed, not locked knees or shifted to one hip.
Breaking the Cycle: Prevention and Management Strategies
Knowing the cause is one thing; fixing it is another. The strategy must be multi-pronged: improve your seated posture, incorporate strategic movement, and support your feet outside of work hours.
Micro-Movements and Scheduled Breaks
Set a timer. Every 30-45 minutes, you must get up. Not just to go to the bathroom, but to move deliberately. Walk to get water, do a quick lap around the house or office, or perform these two critical stretches right at your desk:
- Seated Calf Stretch: While sitting, extend one leg straight. Loop a towel or resistance band around the ball of your foot. Gently pull your toes toward you until you feel a stretch in your calf. Hold 30 seconds. Repeat 3x per leg.
- Toe Pulls / “Toe Yoga”: Sitting or standing, spread your toes wide, then curl them under. This directly mobilizes the plantar fascia.
These micro-breaks reset the tissue length and promote blood flow. It’s the single most effective thing you can do.
Footwear and “At-Home Shoes”
Invest in a great pair of supportive shoes for your home. Brands like Hoka, Brooks, or New Balance with good arch support and cushioned heels are popular. Wear them during your work breaks, when walking around the house, and certainly if you use a standing desk. Do not walk barefoot on tile, hardwood, or concrete. This includes first thing in the morning. Keep a pair of supportive sandals (like Oofos or Chaco) by your bed to slip on before your feet hit the floor. This initial support can make the difference between a manageable morning and a painful one. If you have a dedicated home workspace, consider a small area rug for cushioning, but remember, shoes are best.
Night Splints and Morning Routines
For those with severe morning pain, a night splint can be a game-changer. It’s a brace that holds your foot at a 90-degree angle while you sleep, preventing the plantar fascia and calves from tightening overnight. This means your first steps in the morning are less traumatic. Couple this with a morning routine: before getting out of bed, do your seated calf stretches and gently roll your feet over a frozen water bottle or a lacrosse ball (a form of myofascial release) to reduce inflammation and “wake up” the tissue.
Strengthening for Long-Term Resilience
Stretching is for tightness; strengthening is for resilience. Weak foot intrinsic muscles (the small muscles in the sole) can overload the plantar fascia. Simple exercises like:
- Towel Scrunches: Place a towel on the floor. Use your toes to scrunch it toward you.
- Calf Raises: Slow, controlled raises on both legs, then single-leg, build strength in the entire lower leg support system.
Do these daily, not just when in pain. A strong, resilient foot is less likely to succumb to the stresses of a sedentary job.
When to Worry: Red Flags and Professional Diagnosis
Not all heel pain is plantar fasciitis. It’s important to get a proper diagnosis, especially if your pain is sudden, accompanied by swelling, redness, or a tingling/numbing sensation. Conditions like stress fractures, nerve entrapment (tarsal tunnel), or Achilles tendonitis can mimic the symptoms. A doctor or physical therapist can perform tests and possibly an ultrasound to confirm inflammation of the plantar fascia. If your pain persists for more than two weeks despite aggressive home care (rest, ice, stretching, proper footwear), it’s time to seek professional help. They can provide targeted treatments like custom orthotics, more advanced physical therapy, shockwave therapy, or, in rare chronic cases, discuss other options. They can also assess your specific sitting posture and workstation to give you personalized advice.
Conclusion: It’s About Mindful Movement, Not Just Avoiding Chairs
The link between sitting at a desk and plantar fasciitis is a powerful reminder that our bodies are interconnected systems, and modern habits can have unexpected consequences. Your desk job doesn’t have to sentence you to a lifetime of heel pain. The solution is not to abandon your chair, but to become a strategic, mindful sitter and mover. By optimizing your ergonomic setup to keep your feet in a neutral, supported position, committing to frequent movement breaks with targeted stretches, and supporting your feet with proper footwear even at home, you break the cycle of tightness and overload. You transform your workstation from a potential injury trap into a space that supports your long-term musculoskeletal health. Listen to your body’s early signals—that stiffness after sitting is your cue to move. Start today, make these small adjustments, and give your feet the freedom they need to carry you pain-free for years to come, whether you’re chasing deadlines or chasing dreams.
Frequently Asked Questions
Can I definitely get plantar fasciitis just from sitting at a desk?
Sitting itself isn’t the direct cause, but prolonged, poor-quality sitting with bad posture and lack of movement is a major contributing factor. It creates the tightness and weakness that leads to the condition when you do stand and walk.
What is the single most important thing I can change in my home office?
Ensuring your chair height allows your feet to rest flat on the floor (or on a supportive footrest) with knees at a 90-degree angle. This neutral ankle position prevents the calf and plantar fascia from being held in a shortened state.
Should I wear shoes while working at my desk?
Yes, especially if you feel any heel stiffness or pain. Wear supportive “at-home” shoes or sandals to maintain arch support. If you use a standing desk, supportive footwear is absolutely essential. Avoid going barefoot on hard surfaces during work hours.
How often should I take breaks to prevent this?
Aim for a short, 2-3 minute break every 30-45 minutes. Use this time to stand, walk, and perform your seated calf stretches. Consistency is far more effective than one long break at the end of the day.
Is a standing desk a better solution than sitting?
Not inherently. Standing still for hours is also harmful. The ideal is a sit-stand desk that allows you to alternate between sitting and standing throughout the day, with movement in both positions. Always wear shoes when standing.
When should I see a doctor about my heel pain?
See a doctor or physical therapist if the pain is severe, doesn’t improve after 2 weeks of diligent home care (stretching, proper footwear, ice), or if you have swelling, redness, or numbness. They can confirm the diagnosis and rule out other conditions.